Abstract
Purpose
The aetiology of intestinal barrier dysfunction in Crohn’s disease (CD) is poorly understood. Associations in relatives of CD families suggest a genetic basis, but the relevant variants are still unknown. We hypothesized that variants in genes occurring in pathways such as autophagy and IL23 signalling might contribute to CD by altering intestinal permeability.
Methods
We analysed five variants (rs10758669 within JAK2, rs744166 within STAT3, rs4958847, rs11747270 and rs13361189 within IRGM) in adult German inflammatory bowel disease patients (CD, n = 464; ulcerative colitis (UC), n = 292) and matched healthy controls (n = 508). These data were correlated with gastrointestinal permeability as assessed by lactulose/mannitol ratio in CD patients (n = 141) in remission.
Results
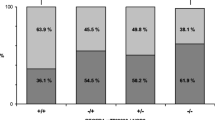
Our data confirm the association between JAK2 rs10758669 (p = 0.026, OR = 1.25, 95% CI = 1.04–1.50) and STAT3 rs744166 (p = 0.04, OR = 0.83, 95% CI = 0.688–0.998) with CD, but not UC. With respect to all the analysed IRGM variants, no association was found to either CD or UC. Among CD patients, an increased intestinal permeability was detected in 65 out of 141 patients (46.1%). Most importantly, patients carrying the C risk allele within JAK2 rs10758669 displayed an increased permeability more often compared with patients without the C allele (p = 0.004). No association with intestinal permeability was found for STAT3 rs744166 and all IRGM variants.
Conclusions
JAK2 rs10758669 and STAT3 rs744166 increase susceptibility for CD. We show that the A>C substitution in rs10758669 of the JAK2 gene is associated with increased intestinal permeability. Altering intestinal barrier function might thus be one mechanism how JAK2 contributes to CD pathogenesis.


Similar content being viewed by others
References
Katz KD, Hollander D, Vadheim CM et al (1989) Intestinal permeability in patients with Crohn’s disease and their healthy relatives. Gastroenterology 97(4):927–931
Teahon K, Smethurst P, Levi AJ et al (1992) Intestinal permeability in patients with Crohn’s disease and their first degree relatives. Gut 33(3):320–323
Hollander D (1993) Permeability in Crohn’s disease: altered barrier functions in healthy relatives? Gastroenterology 104(6):1848–1851
May GR, Sutherland LR, Meddings JB (1993) Is small intestinal permeability really increased in relatives of patients with Crohn’s disease? Gastroenterology 104(6):1627–1632
Wyatt J, Vogelsang H, Hubl W et al (1993) Intestinal permeability and the prediction of relapse in Crohn’s disease. Lancet 341(8858):1437–1439
Yacyshyn BR, Meddings JB (1995) CD45RO expression on circulating CD19+ B cells in Crohn’s disease correlates with intestinal permeability. Gastroenterology 108(1):132–137
Peeters M, Geypens B, Claus D et al (1997) Clustering of increased small intestinal permeability in families with Crohn’s disease. Gastroenterology 113(3):802–807
Soderholm JD, Olaison G, Lindberg E et al (1999) Different intestinal permeability patterns in relatives and spouses of patients with Crohn’s disease: an inherited defect in mucosal defence? Gut 44(1):96–100
Irvine EJ, Marshall JK (2000) Increased intestinal permeability precedes the onset of Crohn’s disease in a subject with familial risk. Gastroenterology 119(6):1740–1744
Beisner J, Stange EF, Wehkamp J (2010) Innate antimicrobial immunity in inflammatory bowel diseases. Expert Rev Clin Immunol 6(5):809–818
Buhner S, Buning C, Genschel J et al (2006) Genetic basis for increased intestinal permeability in families with Crohn’s disease: role of CARD15 3020insC mutation? Gut 55(3):342–347
Barrett JC, Hansoul S, Nicolae DL et al (2008) Genome-wide association defines more than 30 distinct susceptibility loci for Crohn’s disease. Nat Genet 40(8):955–962
Craddock N, Hurles ME, Cardin N et al (2010) Genome-wide association study of CNVs in 16,000 cases of eight common diseases and 3,000 shared controls. Nature 464(7289):713–720
Xavier RJ, Huett A, Rioux JD (2008) Autophagy as an important process in gut homeostasis and Crohn’s disease pathogenesis. Gut 57(6):717–720
Dignass A, Van Assche G, Lindsay JO et al (2010) ECCO The second European evidence-based consensus on the diagnosis and management of Crohn’s disease: current management. J Crohn’s Colitis 4:28–62
Gasche C, Scholmerich J, Brynskov J et al (2000) A simple classification of Crohn’s disease: report of the Working Party for the World Congresses of Gastroenterology, Vienna 1998. Inflamm Bowel Dis 6(1):8–15
Buning C, Molnar T, Nagy F et al (2005) NOD2/CARD15 gene polymorphism in patients with inflammatory bowel disease: is Hungary different? World J Gastroenterol 11(3):407–411
Buhner S, Reese I, Kuehl F et al (2004) Pseudoallergic reactions in chronic urticaria are associated with altered gastroduodenal permeability. Allergy 59(10):1118–1123
Brand S (2009) Crohn’s disease: Th1, Th17 or both? The change of a paradigm: new immunological and genetic insights implicate Th17 cells in the pathogenesis of Crohn’s disease. Gut 58(8):1152–1167
Murray PJ (2007) The JAK-STAT signaling pathway: input and output integration. J Immunol 178(5):2623–2629
Parham C, Chirica M, Timans J et al (2002) A receptor for the heterodimeric cytokine IL-23 is composed of IL-12Rbeta1 and a novel cytokine receptor subunit, IL-23R. J Immunol 168(11):5699–5708
Cargill M, Schrodi SJ, Chang M et al (2007) A large-scale genetic association study confirms IL12B and leads to the identification of IL23R as psoriasis-risk genes. Am J Hum Genet 80(2):273–290
Liu Y, Helms C, Liao W et al (2008) A genome-wide association study of psoriasis and psoriatic arthritis identifies new disease loci. PLoS Genet 4(3):e1000041
Reveille JD, Sims AM, Danoy P et al (2010) Genome-wide association study of ankylosing spondylitis identifies non-MHC susceptibility loci. Nat Genet 42(2):123–127
Al-Sadi R, Ye D, Said HM et al (2010) IL-1beta-induced increase in intestinal epithelial tight junction permeability is mediated by MEKK-1 activation of canonical NF-kappaB pathway. Am J Pathol 177(5):2310–2322
Soderholm JD, Streutker C, Yang PC et al (2004) Increased epithelial uptake of protein antigens in the ileum of Crohn’s disease mediated by tumour necrosis factor alpha. Gut 53(12):1817–1824
MacDonald TT, Hutchings P, Choy MY et al (1990) Tumour necrosis factor-alpha and interferon-gamma production measured at the single cell level in normal and inflamed human intestine. Clin Exp Immunol 81(2):301–305
Ma TY, Iwamoto GK, Hoa NT et al (2004) TNF-alpha-induced increase in intestinal epithelial tight junction permeability requires NF-kappa B activation. Am J Physiol Gastrointest Liver Physiol 286(3):G367–G376
Scharl M, Paul G, Weber A et al (2009) Protection of epithelial barrier function by the Crohn’s disease associated gene protein tyrosine phosphatase n2. Gastroenterology 137(6):2030–2040 e5
Salim SY, Soderholm JD (2011) Importance of disrupted intestinal barrier in inflammatory bowel diseases. Inflamm Bowel Dis 17(1):362–381
Fiocchi C (1998) Inflammatory bowel disease: etiology and pathogenesis. Gastroenterology 115(1):182–205
Podolsky DK (2002) Inflammatory bowel disease. N Engl J Med 347(6):417–429
Xavier RJ, Podolsky DK (2007) Unravelling the pathogenesis of inflammatory bowel disease. Nature 448(7152):427–434
Cuthbert AP, Fisher SA, Mirza MM et al (2002) The contribution of NOD2 gene mutation to the risk and site of disease in inflammatory bowel disease. Gastroenterology 122:867–874
Hampe J, Franke A, Rosenstiel P et al (2007) A genome-wide association scan of nonsynonymous SNPs identifies a susceptibility variant for Crohn disease in ATG16L1. Nat Genet 39(2):207–211
Wehkamp J, Stange EF (2010) Paneth’s disease. J Crohn’s Colitis 4:523–531
Ferguson LR, Han DY, Fraser AG et al (2010) Genetic factors in chronic inflammation: Single nucleotide polymorphisms in the STAT-JAK pathway, susceptibility to DNA damage and Crohn’s disease in a New Zealand population. Mutat Res 690(1–2):108–115
Sato K, Shiota M, Fukuda S et al (2009) Strong evidence of a combination polymorphism of the tyrosine kinase 2 gene and the signal transducer and activator of transcription 3 gene as a DNA-based biomarker for susceptibility to Crohn’s disease in the Japanese population. J Clin Immunol 29(6):815–825
Anderson CA, Massey DC, Barrett JC et al (2009) Investigation of Crohn’s disease risk loci in ulcerative colitis further defines their molecular relationship. Gastroenterology 136(2):523–529 e3
Franke A, Balschun T, Karlsen TH et al (2008) Replication of signals from recent studies of Crohn’s disease identifies previously unknown disease loci for ulcerative colitis. Nat Genet 40(6):713–715
McCarroll SA, Huett A, Kuballa P et al (2008) Deletion polymorphism upstream of IRGM associated with altered IRGM expression and Crohn’s disease. Nat Genet 40(9):1107–1112
Singh SB, Davis AS, Taylor GA et al (2006) Human IRGM induces autophagy to eliminate intracellular mycobacteria. Science 313(5792):1438–1441
Weersma RK, Stokkers PC, Cleynen I et al (2009) Confirmation of multiple Crohn’s disease susceptibility loci in a large Dutch–Belgian cohort. Am J Gastroenterol 104(3):630–638
Latiano A, Palmieri O, Cucchiara S et al (2009) Polymorphism of the IRGM gene might predispose to fistulizing behavior in Crohn’s disease. Am J Gastroenterol 104(1):110–116
Yamazaki K, Takahashi A, Takazoe M et al (2009) Positive association of genetic variants in the upstream region of NKX2-3 with Crohn’s disease in Japanese patients. Gut 58(2):228–232
Prescott NJ, Dominy KM, Kubo M et al (2010) Independent and population-specific association of risk variants at the IRGM locus with Crohn’s disease. Hum Mol Genet 19(9):1828–1839
Büning C, Durmus T, Molnar T et al (2007) A study in three European IBD cohorts confirms that the ATG16L1 c.898A>G (p.Thr300Ala) variant is a susceptibility factor for Crohn’s disease. J Crohn’s Colitis 1:70–76
Acknowledgement
The study was supported by a grant from the Eli and Edythe Broad Foundation (to C.B., Proposal No. IBD-0164R), by a grant of the German Ministry for Education and Research (BMBF)—Competence Network “Inflammatory Bowel Disease”: 01GI0284 TP 1.17 and by the Forschungsförderung of the Charité, Universitätsmedizin Berlin. We thank all patients who participated in this evaluation.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Prager, M., Büttner, J., Haas, V. et al. The JAK2 variant rs10758669 in Crohn’s disease: altering the intestinal barrier as one mechanism of action. Int J Colorectal Dis 27, 565–573 (2012). https://doi.org/10.1007/s00384-011-1345-y
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-011-1345-y