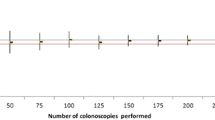
The success rate for reaching the cecum has been widely discussed as an indicatorof technical expertise for colonoscopy. However, few studies have addressed the impact of endoscopist-specific parameters on cecal intubation rates. The aim of this study wasto characterize the relationship between endoscopist-specific parameters (age, gender, experience level, annual procedure volume, insertion and withdrawal times) and cecal intubation rates for colonoscopy. Procedural data from all colonoscopies performed by gastroenterologists at the outpatient endoscopy unit of Rochester Methodist Hospital, Minnesota, between January and December 2003 were reviewed. Procedural data of 45 endoscopists who performed 17,100 colonoscopies over the study period were analyzed. The average cecal intubation rate was 93.9% (SD, 2.9%). Higher experience level (> 9 years [median]) was significantly predictive of a cecal intubation rate > 94% (OR = 3.43; 95% CI, 1.03–12.29; P = 0.04). Although higher procedure volume was not predictive of higher colonoscopy completion rates overall, when analysis was confined to the junior faculty members (< 5 years’ experience), completion rates for those endoscopists doing > 200 per year (92.5%) was significantly higher than for those doing < 200 per year (88.5%; P = 0.04). Our observations suggest that cecal intubation rates increase with increasing endoscopist experience. Moreover, among junior endoscopists, an annual volume of at least 200 procedures appears to be required to maintain adequate competence. Future prospective studies should provide data to support consensus guidelines recommending minimum annual procedure numbers required for maintenance of endoscopic competence among trained endoscopists.
Similar content being viewed by others
References
Mandel JS, Bond JH, Church TR, Snover DC, Bradley GM, Schuman LM, Ederer F: Reducing mortality from colorectal cancer by screening for fecal occult blood. Minnesota Colon Cancer Control Study. N Engl J Med 328(19):1365–1371, 1993
Hardcastle JD, Chamberlain JO, Robinson MH, Moss SM, Amar SS, Balfour TW, James PD, Mangham CM: Randomised controlled trial of faecal-occult-blood screening for colorectal cancer. Lancet 348(9040):1472–1477, 1996
Kronborg O, Fenger C, Olsen J, Jorgensen OD, Sondergaard O: Randomised study of screening for colorectal cancer with faecal-occult-blood test. Lancet 348(9040):1467–1471, 1996
Selby JV, Friedman GD, Quesenberry CP Jr, Weiss NS: A case-control study of screening sigmoidoscopy and mortality from colorectal cancer. N Engl J Med 326(10):653–657, 1992
Newcomb PA, Norfleet RG, Storer BE, Surawicz TS, Marcus PM: Screening sigmoidoscopy and colorectal cancer mortality. J Natl Cancer Inst 84(20):1572–1575, 1992
Lieberman DA, Weiss DG, Bond JH, Ahnen DJ, Garewal H, Chejfec G: Use of colonoscopy to screen asymptomatic adults for colorectal cancer. Veterans Affairs Cooperative Study Group 380. N Engl J Med 343(3):162–168, 2000
Imperiale TF, Wagner DR, Lin CY, Larkin GN, Rogge JD, Ransohoff DF: Risk of advanced proximal neoplasms in asymptomatic adults according to the distal colorectal findings. N Engl J Med 343(3):169–174, 2000
Harewood GC, Lieberman DA: Colonoscopy practice patterns since introduction of Medicare coverage for average-risk screening. Clin Gastroenterol Hepatol 2(1):72–77, 2004
Prajapati DN, Saeian K, Binion DG, Staff DM, Kim JP, Massey BT, Hogan WJ: Volume and yield of screening colonoscopy at a tertiary medical center after change in medicare reimbursement. Am J Gastroenterol 98(1):194–199, 2003
Rex DK, Bond JH, Winawer S, Levin TR, Burt RW, Johnson DA, Kirk LM, Litin S, Lieberman DA, Waye JD, Church J, Marshall JB, Riddell RH: Quality in the technical performance of colonoscopy and the continuous quality improvement process for colonoscopy: recommendations of the U.S. Multi-Society Task Force on Colorectal Cancer. Am J Gastroenterol 97(6):1296–1308, 2002
Chak A, Cooper GS, Blades EW, Canto M, Sivak MV Jr: Prospective assessment of colonoscopic intubation skills in trainees. Gastrointest Endosc 44(1):54–57, 1996
Marshall JB, Barthel JS: The frequency of total colonoscopy and terminal ileal intubation in the 1990s. Gastrointest Endosc 39(4):518–520, 1993
Waye JD, Bashkoff E: Total colonoscopy: Is it always possible?. Gastrointest Endosc 37(2):152–154, 1991
Melton LJ 3rd: History of the Rochester Epidemiology Project. Mayo Clin Proc 71(3):266–274, 1996
Saunders BP, Fukumoto M, Halligan S, Jobling C, Moussa ME, Bartram CI, Williams CB: Why is colonoscopy more difficult in women?. Gastrointest Endosc 43(2, Pt 1):124–126,1996
Webb WA: Colonoscoping the “difficult” colon. Am Surg 57(3):178–182, 1991
Church J: Complete colonoscopy: How often, and if not, why not?. Am J Gastroenterol 87:1320, 1992 (abstr)
Blades EW, Chak A: Effect of previous surgery on performance of colonoscopy. Am J Gastroenterol 88:1567, 1993 (abstr)
Demartino P, Conn, M., Allen M: Factors influencing time to cecum during colonoscopy. Am J Gastroenterol 88:1572, 1993 (abstr)
Marshall JB, Barthel JS: The frequency of total colonoscopy and terminal ileal intubation in the 1990s. Gastrointest Endosc 39(4):518–520, 1993
ASGE: Principles of Training in GI Endoscopy. Manchester, MA, Standards of Training Committee, American Society for Gastrointestinal Endoscopy, 1991
Cotton PB, Connor P, McGee D, Jowell P, Nickl N, Schutz S, Leung J, Lee J, Libby E: Colonoscopy: practice variation among 69 hospital-based endoscopists. Gastrointest Endosc 57(3):352–357, 2003
Singhvi S, Small, P, Bell, GD, Pearson J, Boobis L, Crighton I: Audit of colonoscopy in a large DGH: implications for trainers and trainees of the JAG recommendations. Gut 46:A15, 2000 (abstr)
Robinson J, Small P, Bell GD, Crighton I,Corson J, Hancock J: A prospective audit of colonoscopy in a large DGH—Factors effecting caecal intubation rates. Gut 48:A10, 2001 (abstr)
Bowles CJA, Leicester R, Swarbrick E, Williams CB, Romaya C, Epstein O: Intercollegiate—BSG National Colonoscopy Audit: methods used to identify the caecum and caecal intubation rate. Gut 48:A10–A11, 2001
Bowles CJ, Leicester R, Romaya C, Swarbrick E, Williams CB, Epstein O: A prospective study of colonoscopy practice in the UK today: Are we adequately prepared for national colorectal cancer screening tomorrow?. Gut 53(2):277–283, 2004
Rex DK: Colonoscopy practice variation. Gastrointest Endosc 58(4):639–640, 2003
Cirocco WC, Rusin LC: Confirmation of cecal intubation during colonoscopy. Dis Colon Rectum 38(4):402–406, 1995
Marshall JB, Brown DN: Photodocumentation of total colonoscopy: How successful are endoscopists? Do reviewers agree? Gastrointest Endosc 44(3):243–248, 1996
Rex DK: Effect of variable stiffness colonoscopes on cecal intubation times for routine colonoscopy by an experienced examiner in sedated patients. Endoscopy 33(1):60–64, 2001
Howell DA, Ku PM, Desilets DJ, Campana JM: A comparative trial of variable stiffness colonoscopes. Gastointest Endosc 51:AB179, 2000 (abstr)
Gostout CJ, Sorbi D, Knipshield MA: Variable rigidity colonoscopes: A prospective, randomized controlled study. Gastointest Endosc 53:AB179, 2001 (abstr)
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Harewood, G.C. Relationship of Colonoscopy Completion Rates and Endoscopist Features. Dig Dis Sci 50, 47–51 (2005). https://doi.org/10.1007/s10620-005-1276-y
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/s10620-005-1276-y