Abstract
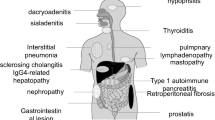
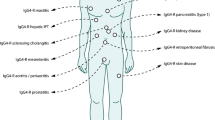
Recent studies suggested the existence of two subtypes of autoimmune pancreatitis (AIP): type 1 related with IgG4 (lymphoplasmacytic sclerosing pancreatitis; LPSP) and type 2 related with a granulocytic epithelial lesion (idiopathic duct-centric chronic pancreatitis; IDCP). Apart from type 2 AIP, the pathological features of type 1 AIP with increased serum IgG4/IgE levels, abundant infiltration of IgG4+ plasmacytes and lymphocytes, fibrosis, and steroid responsiveness are suggestive of abnormal immunity such as allergy or autoimmunity. Moreover, the patients with type 1 AIP often have extrapancreatic lesions such as sclerosing cholangitis, sclerosing sialadenitis, or retroperitoneal fibrosis showing similar pathological features. Based on these findings, many synonyms have been proposed for these conditions, such as “multifocal idiopathic fibrosclerosis”, “IgG4-related autoimmune disease”, “IgG4-related sclerosing disease”, “IgG4-related plasmacytic disease”, and “IgG4-related multiorgan lymphoproliferative syndrome”, all of which may refer to the same conditions. Therefore, the Japanese Research Committee for “Systemic IgG4-related Sclerosing Disease” proposed a disease concept and clinical diagnostic criteria based on the concept of multifocal fibrosclerosis in 2009, in which the term “IgG4-related disease” was appointed as a minimal consensus on these conditions. Although the significance of IgG4 in the development of “IgG4-related disease” remains unclear, we have proposed a hypothesis for the development of type 1 AIP, one of the IgG4-related disease. The concept and diagnostic criteria of “IgG4-related disease” will be changed in accordance with future studies.





Similar content being viewed by others
Abbreviations
- AIP:
-
Autoimmune pancreatitis
- ANA:
-
Anti-nuclear antibody
- CA-II:
-
Carbonic anhydrase-II
- CTLA-4 :
-
Cytotoxic T lymphocyte antigen-4
- ERCP:
-
Endoscopic retrograde cholangiopancreatography
- FCRL:
-
Fc-receptor-like
- IFN-γ:
-
Interferon-γ
- IL-4:
-
Interleukin-4
- LF:
-
Lactoferrin
- LPSP:
-
Lymphoplasmacytic sclerosing pancreatitis
- MD:
-
Mikulicz disease
- MHC:
-
Major histocompatibility complex
- MOLPS:
-
Multiorgan lymphoproliferative disease
- PBP:
-
Plasminogen-binding protein
- SjS:
-
Sjögren’s syndrome
- PSC:
-
Primary sclerosing cholangitis
- RF:
-
Rheumatoid factor
- SIPS:
-
IgG4-systemic plasmacytic syndrome
- SLE:
-
Systemic lupus erythematosus
- Treg:
-
Regulatory T cell
- UBR2:
-
Ubiquitin-protein ligase E3 component n-recognin 2
References
Sarles H, Sarles JC, Muratore R, Guien C (1961) Chronic inflammatory sclerosis of the pancreas—an autonomous pancreatic disease? Am J Dig Dis 6:688–698
Yoshida K, Toki F, Takeuchi T, Watanabe S, Shiratori K, Hayashi N (1995) Chronic pancreatitis caused by an autoimmune abnormality. Proposal of the concept of autoimmune pancreatitis. Dig Dis Sci 40:1561–1568
Hamano H, Kawa S, Horiuchi A et al (1995) High serum IgG4 concentrations in patients with sclerosing pancreatitis. New Engl J Med 344:732–738
Okazaki K, Uchida K, Chiba T (2001) Recent concept of autoimmune-related pancreatitis. J Gastroenterol 36:293–302
Okazaki K (2006) Autoimmune pancreatitis—recent concept. In: Parviz M (ed) Target organ toxicology series, Toxicology of the pancreas. Taylor & Francis, Boca Raton, pp 59–73
Pickartz T, Mayerle J, Lerch M (2007) Autoimmune pancreatitis. Nat Clin Pract Gastroenterol Hepatol 4:314–323
Kawaguchi K, Koike M, Tsuruta K, Okamoto A, Tabata I, Fujita N (1991) Lymphoplasmacytic sclerosing pancreatitis with cholangitis: a variant of primary sclerosing cholangitis extensively involving pancreas. Hum Pathol 22:387–395
Kamisawa T, Funata N, Hayashi Y et al (2003) A new clinicopathological entity of IgG4-related autoimmune disease. J Gastroenterol 38:982–984
Comings DE et al (1967) Familial multifocal fibrosclerosis. Ann Intern Med 66:884–892
Chari ST, Kloeppel G, Zhang L et al (2010) Histopathologic and clinical subtypes of autoimmune pancreatitis: the Honolulu consensus document. Pancreas 39:549–554
Mikulicz J (1892) Über eine eigenartige symmetrishe Erkrankung der Tränen und Mundspeicheldrüsen. Beitr z Chir Fesrschr f Theodor Billroth, Stuttgart, pp 610–630
Okazaki K, Kawa S, Kamisawa T et al (2006) Clinical diagnostic criteria of autoimmune pancreatitis: revised proposal. J Gastroenterol 41:626–631
Kamisawa T, Okamoto A (2006) Autoimmune pancreatitis: proposal of IgG4-related sclerosing disease. J Gastroenterol 41:613–625
Yamamoto M, Takahashi H, Ohara M et al (2006) A new conceptualization for Mikulicz’s disease as an IgG4-related plasmacytic disease. Mod Rheumatol 16:335–340
Masaki Y, Dong L, Kurose N et al (2009) Proposal for a new clinical entity, IgG4-positive multi-organ lymphoproliferative syndrome: analysis of 64 cases of IgG4-related disorders. Ann Rheum Dis 68:1310–1315
Notohara K, Burgart LJ, Yadav D et al (2003) Idiopathic chronic pancreatitis with periductal lymphoplasmacytic infiltration: clinico-pathologic features of 35 cases. Am J Surg Pathol 27:1119–1127
Zamboni G, Lüttges J, Capelli P et al (2004) Histopathological features of diagnostic and clinical relevance in autoimmune pancreatitis: a study on 53 resection specimens and 9 biopsy specimens. Virchows Arch 445:552–563
Kamisawa T, Funata N, Hayashi Y et al (2003) Close relationship between autoimmune pancreatitis and multifocal fibrosclerosis. Gut 52:683–687
Saegusa H, Momose M, Kawa S et al (2003) Hilar and pancreatic gallium-67 accumulation is characteristic feature of autoimmune pancreatitis. Pancreas 27:20–251
Erkelens GW, Vleggaar FP, Lesterhuis W et al (1999) Sclerosing pancreato-cholangitis responsive to steroid therapy. Lancet 354:43–44
Nakazawa T, Ohara H, Yamada T (2001) Atypical primary sclerosing cholangitis cases associated with unusual pancreatitis. Hepatogastroenterology 48:625–630
Hamano H, Kawa S, Ochi Y et al (2002) Hydronephrosis associated with retroperitoneal fibrosis and sclerosing pancreatitis. Lancet 359:1403–1404
Takeda S, Haratake J, Kasai T et al (2004) IgG4-associated idiopathic tubulointerstitial nephritis complicating autoimmune pancreatitis. Nephrol Dial Transplant 19:474–476
Uchiyama-Tanaka Y, Mori Y, Kimura T et al (2004) Acute tubulointerstitial nephritis associated with autoimmune-related pancreatitis. Am J Kidney Dis 43:e18–e25
Shimatsu A, Oki Y, Fujisawa I et al (2009) Pituitary and stalk lesions (infundibulo-hypophysitis) associated with immunoglobulin G4-related systemic disease: an emerging clinical entity. Endocr J 56:1033–1041
Komatsu K, Hamano H, Ochi Y et al (2005) High prevalence of hypothyroidism in patients with autoimmune pancreatitis. Dig Dis Sci 50:1052–1057
Yoshimura Y, Takeda S, Ieki Y et al (2006) IgG4-associated prostatitis complicating autoimmune pancreatitis. Intern Med 45:897–901
Okazaki K, Uchida K, Matsushita M et al (2007) How to diagnose autoimmune pancreatitis by the revised Japanese clinical criteria. J Gastroenterol 42(Suppl 18):32–38
Ohara H, Nakazawa T, Sano H et al (2005) Systemic extrapancreatic lesions associated with autoimmune pancreatitis. Pancreas 31:232–237
Hamano H, Arakura N, Muraki T et al (2006) Prevalence and distribution of extrapancreatic lesions complicating autoimmune pancreatitis. J Gastroenterol 41:1197–1205
Kawa S, Okazaki K, Kamisawa T et al (2010) Japanese consensus guidelines for management of autoimmune pancreatitis: II. Extrapancreatic lesions, differential diagnosis. J Gastroenterol 45:355–369
Okazaki K, Kawa S, Kamisawa T et al (2009) Japanese clinical guidelines for autoimmune pancreatitis. Pancreas 38:849–866
Okazaki K, Kawa S, Kamisawa T et al (2010) Japanese consensus guidelines for management of autoimmune pancreatitis: I. Concept and diagnosis of autoimmune pancreatitis. J Gastroenterol 45:249–265
Kamisawa T, Okazaki K, Kawa S et al (2010) Japanese consensus guidelines for management of autoimmune pancreatitis: III. Treatment and prognosis of AIP. J Gastroenterol 45:471–477
Okazaki K, Uchida K, Research Committee Members (2009) Proposal of the concept and diagnostic criteria of IgG4-related disease. Annual reports of research committee of intractable diseases supported by Ministry of Health, Labour and Welfare of Japan, pp 25–30 (in Japanese)
Masaki Y, Sugai S, Umehara H (2010) IgG4-related diseases including Mikulicz’s disease and sclerosing pancreatitis: diagnostic insights. J Rheumatol 37:1380–1385
Kawa S, Ota M, Yoshizawa K et al (2002) HLA DRB10405-DQB10401 haplotype is associated with autoimmune pancreatitis in the Japanese population. Gastroenterology 122:1264–1269
Park do H, Kim MH, Oh HB (2008) Substitution of aspartic acid at position 57 of the DQbeta1 affects relapse of autoimmune pancreatitis. Gastroenterology 134:440–446
Kochi Y, Yamada R, Suzuki A et al (2005) A functional variant in FCRL3, encoding Fc receptor-like 3, is associated with rheumatoid arthritis and several autoimmunities. Nat Genet 37(5):478–485
Umemura T, Ota M, Hamano H, Katsuyama Y, Kiyosawa K, Kawa S (2006) Genetic association of Fc receptor-like 3 polymorphisms with autoimmune pancreatitis in Japanese patients. Gut 55(9):1367–1368
Umemura T, Katsuyama Y, Hamano H et al (2009) Association analysis of Toll-like receptor 4 polymorphisms with autoimmune pancreatitis. Hum Immunol 70:742–746
Chang MC, Chang YT, Tien YW et al (2007) T-cell regulatory gene CTLA-4 polymorphism/haplotype association with autoimmune pancreatitis. Clin Chem 53(9):1700–1705
Umemura T, Ota M, Hamano H et al (2008) Association of autoimmune pancreatitis with cytotoxic T-lymphocyte antigen 4 gene polymorphisms in Japanese patients. Am J Gastroenterol 103(3):588–594
Ueda H, Howson JM, Esposito L et al (2003) Association of the T-cell regulatory gene CTLA4 with susceptibility to autoimmune disease. Nature 423(6939):506–511
Roitt I (1997) Antibodies. In: Roitt I (ed) Roitt’s essential immunology, 9th edn. Blackwell Science, London, pp 43–62
Taguchi M, Kihara Y, Nagashio Y, Yamamoto M, Otsuki M, Harada M (2009) Decreased production of immunoglobulin M and A in autoimmune pancreatitis. J Gastroenterol 44:1133–1139
Robinson DS, Larche M, Durham SR (2004) Tregs and allergic disease. J Clin Invest 114(10):1389–1397
van der Neut Kolfschoten M, Schuurman J, Losen M et al (2007) Anti-inflammatory activity of human IgG4 antibodies by dynamic Fab arm exchange. Science 317(5844):1554–1557
Kawa S, Kitahara K, Hamano H et al (2008) A novel immunoglobulin-immunoglobulin interaction in autoimmunity. PLoS ONE 3(2):e1637
Cornell LD, Chicano SL, Deshpande V et al (2007) Pseudotumors due to IgG4 immune-complex tubulointerstitial nephritis associated with autoimmune pancreatocentric disease. Am J Surg Pathol 31(10):1586–1597
Muraki T, Hamano H, Ochi Y et al (2006) Autoimmune pancreatitis and complement activation system. Pancreas 32(1):16–21
Uchida K, Okazaki K, Konishi Y et al (2000) Clinical analysis of autoimmune-related pancreatitis. Am J Gastroenterol 95(10):2788–2794
Okazaki K, Uchida K, Ohana M et al (2000) Autoimmune-related pancreatitis is associated with autoantibodies and a Th1/Th2-type cellular immune response. Gastroenterology 118(3):573–581
Nishi H, Tojo A, Onozato ML et al (2007) Anti-carbonic anhydrase II antibody in autoimmune pancreatitis and tubulointerstitial nephritis. Nephrol Dial Transplant 22(4):1273–1275
Aparisi L, Farre A, Gomez-Cambronero L et al (2005) Antibodies to carbonic anhydrase and IgG4 levels in idiopathic chronic pancreatitis: relevance for diagnosis of autoimmune pancreatitis. Gut 54(5):703–709
Nishimori I, Miyaji E, Morimoto K, Nagao K, Kamada M, Onishi S (2005) Serum antibodies to carbonic anhydrase IV in patients with autoimmune pancreatitis. Gut 54(2):274–281
Asada M, Nishio A, Uchida K et al (2006) Identification of a novel autoantibody against pancreatic secretory trypsin inhibitor in patients with autoimmune pancreatitis. Pancreas 33(1):20–26
Endo T, Takizawa S, Tanaka S et al (2009) Amylase alpha-2A autoantibodies: novel marker of autoimmune pancreatitis and fulminant type 1 diabetes. Diabetes 58(3):732–737
Takizawa S, Endo T, Wanjia X, Tanaka S, Takahashi M, Kobayashi T (2009) HSP 10 is a new autoantigen in both autoimmune pancreatitis and fulminant type 1 diabetes. Biochem Biophys Res Commun 386(1):192–196
Frulloni L, Lunardi C, Simone R et al (2009) Identification of a novel antibody associated with autoimmune pancreatitis. N Engl J Med 361(22):2135–2142
Nishimori I, Bratanova T, Toshkov I et al (1995) Induction of experimental autoimmune sialoadenitis by immunization of PL/J mice with carbonic anhydrase II. J Immunol 154(9):4865–4873
Ueno Y, Ishii M, Takahashi S, Igarashi T, Toyota T, LaRusso NF (1998) Different susceptibility of mice to immune-mediated cholangitis induced by immunization with carbonic anhydrase II. Lab Invest 78(5):629–637
Kountouras J, Zavos C, Gavalas E, Tzilves D (2007) Challenge in the pathogenesis of autoimmune pancreatitis: potential role of helicobacter pylori infection via molecular mimicry. Gastroenterology 133(1):368–369
Kountouras J, Zavos C, Chatzopoulos D (2005) A concept on the role of Helicobacter pylori infection in autoimmune pancreatitis. J Cell Mol Med 9(1):196–207
Guarneri F, Guarneri C, Benvenga S (2005) Helicobacter pylori and autoimmune pancreatitis: role of carbonic anhydrase via molecular mimicry? J Cell Mol Med 9(3):741–744
McGeachy MJ, Cua DJ (2007) The link between IL-23 and Th17 cell-mediated immune pathologies. Semin Immunol 19(6):372–376
Oukka M (2007) Interplay between pathogenic Th17 and regulatory T cells. Ann Rheum Dis 66(Suppl 3):iii87–iii90
Yamamoto M, Harada S, Ohara M et al (2005) Clinical and pathological differences between Mikulicz’s disease and Sjogren’s syndrome. Rheumatology 44(2):227–234
Zen Y, Fujii T, Harada K et al (2007) Th2 and regulatory immune reactions are increased in immunoglobulin G4-related sclerosing pancreatitis and cholangitis. Hepatology 45(6):1538–1546
Uchida K, Okazaki K, Nishi T et al (2002) Experimental immune-mediated pancreatitis in neonatally thymectomized mice immunized with carbonic anhydrase II and lactoferrin. Lab Invest 82(4):411–424
Ajjan RA, McIntosh RS, Waterman EA et al (1998) Analysis of the T-cell receptor Valpha repertoire and cytokine gene expression in Sjogren’s syndrome. Br J Rheumatol 37(2):179–185
Dienes HP, Lohse AW, Gerken G et al (1997) Bile duct epithelia as target cells in primary biliary cirrhosis and primary sclerosing cholangitis. Virchows Arch 431(2):119–124
Valencia X, Lipsky PE (2007) CD4+CD25+FoxP3+ regulatory T cells in autoimmune diseases. Nat Clin Pract Rheumatol 3(11):619–626
Gottenberg JE, Lavie F, Abbed K et al (2005) CD4 CD25high regulatory T cells are not impaired in patients with primary Sjogren’s syndrome. J Autoimmun 24(3):235–242
Miyoshi H, Uchida K, Taniguchi T et al (2008) Circulating naive and CD4+CD25high regulatory T cells in patients with autoimmune pancreatitis. Pancreas 36(2):133–140
Stanley JR, Amagai M (2006) Pemphigus, bullous impetigo, and the staphylococcal scalded-skin syndrome. N Engl J Med 355(17):1800–1810
Fujii H, Nakatani K, Arita N et al (2003) Internalization of antibodies by endothelial cells via fibronectin implicating a novel mechanism in lupus nephritis. Kidney Int 64(5):1662–1670
Aalberse RC, Stapel SO, Schuurman J, Rispens T (2009) Immunoglobulin G4: an odd antibody. Clin Exp Allergy 39(4):469–477
Ruiter B, Knol EF, van Neerven RJ et al (2007) Maintenance of tolerance to cow’s milk in atopic individuals is characterized by high levels of specific immunoglobulin G4. Clin Exp Allergy 37(7):1103–1110
Hussain R, Poindexter RW, Ottesen EA (1992) Control of allergic reactivity in human filariasis. Predominant localization of blocking antibody to the IgG4 subclass. J Immunol 148(9):2731–2737
Yazdanbakhsh M, van den Biggelaar A, Maizels RM (2001) Th2 responses without atopy: immunoregulation in chronic helminth infections and reduced allergic disease. Trends Immunol 22(7):372–377
Sakaguchi S, Fukuma K, Kuribayashi K, Masuda T (1985) Organ-specific autoimmune diseases induced in mice by elimination of T cell subset. I. Evidence for the active participation of T cells in natural self-tolerance; deficit of a T cell subset as a possible cause of autoimmune disease. J Exp Med 161(1):72–87
Demols A, Le Moine O, Desalle F, Quertinmont E, Van Laethem JL, Deviere J (2000) CD4(+)T cells play an important role in acute experimental pancreatitis in mice. Gastroenterology 118(3):582–590
Vallance BA, Hewlett BR, Snider DP, Collins SM (1998) T cell-mediated exocrine pancreatic damage in major histocompatibility complex class II-deficient mice. Gastroenterology 115(4):978–987
Sakaguchi Y, Inaba M, Tsuda M et al (2008) The Wistar Bonn Kobori rat, a unique animal model for autoimmune pancreatitis with extrapancreatic exocrinopathy. Clin Exp Immunol 152(1):1–12
Marth T, Strober W, Kelsall BL (1996) High dose oral tolerance in ovalbumin TCR-transgenic mice: systemic neutralization of IL-12 augments TGF-beta secretion and T cell apoptosis. J Immunol 157(6):2348–2357
Hahm KB, Im YH, Lee C et al (2000) Loss of TGF-beta signaling contributes to autoimmune pancreatitis. J Clin Invest 105(8):1057–1065
Kusuda T, Uchida K, Satoi S et al (2010) Idiopathic duct-centric pancreatitis (IDCP) with immunological studies. Intern Med 49(23):2569–2575
Acknowledgment
This study was partly supported by a Grant-in-Aid for Scientific Research from the Ministry of Culture and Science of Japan (20590810) and a Grant-in-Aid for “Research for Intractable Disease” Program from the Ministry of Health, Labor and Welfare of Japan.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Okazaki, K., Uchida, K., Miyoshi, H. et al. Recent Concepts of Autoimmune Pancreatitis and IgG4-Related Disease. Clinic Rev Allerg Immunol 41, 126–138 (2011). https://doi.org/10.1007/s12016-010-8214-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12016-010-8214-2